Juvenile Huntington’s Disease: The Cruel Mutation
Looking back, signs that Jane Mervar’s husband, Karl, had Huntington’s Disease (HD) started about when their youngest daughter, Karli, began to have trouble paying attention in school. Karl had become abusive, paranoid, and unemployable due to his drunken appearance. The little girl, born in September 1996, was hyperactive and had difficulty following directions. When by age 5 Karli’s left side occasionally stiffened and her movements slowed, Jane began the diagnostic journey that would end with Karli’s diagnosis of HD, which had affected the little girl’s paternal grandmother.
Soon Karli could no longer skip, hop, or jump. And new troubles emerged. ”She had cold sweats, tachycardia, and chronic itching. She fell and suffered chronic pain. By age 6 she was losing her speech and became withdrawn,” Jane recalls. Karli drooled and her speech became unintelligible. By age 7 her weight had plunged, and by 8 she developed pneumonia three times due to difficulty swallowing. By age 9 she required a feeding tube, suffered seizures, and would go long periods without sleep.
AN ADULT’S DISEASE IN A CHILD
This isn’t the way that a disease is supposed to run in families, striking child before parent. HD is regarded as a disease of adulthood, but in fact about 10% of people with the condition are under age 20 – they have juvenile Huntington’s disease (JHD).
“Horse-and-buggy doctor” George Sumner Huntington first described HD in 1872. As a young man he’d accompanied his father and grandfather on house calls in East Hampton, Long Island, where a few local families had a mysterious movement disorder. The youngest Huntington recalled two very thin women gripped by constant contortions, and several men who staggered about as if intoxicated. He later described the symptoms intensifying “until the hapless sufferer is but a quivering wreck of his former self.”

Dr. Huntington deduced the autosomal dominant inheritance pattern of HD. It affects both sexes, with each child of someone with the disease facing a 50:50 chance of sharing the fate. Loss of motor control typically begins in the late thirties, but behavioral and cognitive signs are often present years earlier, sometimes unrecognized. Folksinger Woody Guthrie put a famous face on HD 45 years ago, but the community today needs an Angelina Jolie.
HD symptoms in children differ from those in adults – Karli’s problems in school and stiffness were classic — but inside cells, a similar crisis unfolds in a patient of any age.
The Htt gene encodes the protein huntingtin. The gene normally includes up to 35 copies of the DNA triplet CAG, just before the first exon (protein-encoding part). The disease arises when the gene grows – HD is the quintessential “expanding triplet repeat” disorder. Perhaps the enzymes that replicate DNA as sperm and egg form misalign while duplicating a short repeated sequence, like copying a line in a word document and introducing repeats of a word word word.
The triplet repeat somehow triggers a cascade of destruction, with its most profound effects in the “medium spiny neurons” in the movement centers of the brain. The Htt gene with too many CAGs encodes a protein with too many glutamines. The protein can’t fold properly, sticking to itself and to other proteins, blocking axons in neurons of the brain’s striatum, preventing distribution of essential growth factors. The white matter of the brain shrinks.
Changes in behavior and thinking often precede the constant movements that fascinated the young Dr. Huntington. Irritability, loss of impulse control, and aggression are hallmarks. Jane’s husband Karl spent wildly and threatened his family and others with guns. He spent his final years in a nursing home knowing that social services would take away his daughters otherwise.
AN UNUSUAL MUTATION
Karl was diagnosed six weeks after Karli in 2002. He was 35, she just 6. They died within weeks of each other in early 2010.
But the story gets worse. Karli’s sister Jacey (who founded jhdkids.com), was diagnosed in 2004 at age 13, and her sister Erica in 2007 at age 17. The family history is so complex and unbelievable that even Jane has trouble recalling the chronology. All three girls inheriting the disease is probably just bad luck, but the repeat size for Karli echoes an unusual event.
In HD, gene size matters. Most adults have 40-60 repeats. Karl had 47 and his two older daughters have 47 and 49. But Karli inherited 99 CAGs, a consequence of DNA replication enzymes looping and doubling her father’s 47. It’s little wonder she got sick so fast — longer repeats mean earlier onset.
Most HD kids with very expanded mutations inherit them from their fathers, and this may be due to the different timetables of sperm and egg production. A female at puberty has about 400,000 eggs, each halted on the brink of completing meiosis, when the slippage that expands the gene could happen. But a male shoots out a quarter of a billion sperm with each ejaculation – many chances over a reproductive lifetime for the gene to be miscopied and grow.
WHEN, AND IF, TO TEST
A test to count CAG repeats is essential to confirm a clinical diagnosis of HD. When genetic testing first became available in the mid 1990s, following a decade of using a less-predictive marker test, concern was that people finding out they have the mutation before symptoms begin would freak out. That hasn’t happened. Nor has testing found many takers. Most “at-risk” individuals, those who know they have one affected parent, choose not to be tested.
Because testing raises complicated psychosocial issues, and because onset is usually in the fourth decade, it’s generally not recommended for those under 18. But when the young person has symptoms, it’s a different story.
Martha A. Nance MD, medical director of the Struthers Parkinson’s Center and the director of the HD Center of Excellence at Hennepin County Medical Center, both in Minneapolis, and author of “The Juvenile HD Handbook,” explains the nuances. “It’s important to distinguish diagnostic testing in a child who is having problems from presymptomatic testing in a child whose parent has HD or is at-risk for HD but has no neurologic or psychiatric symptoms.”
Presymptomatic testing doesn’t make much sense, Dr. Nance says. “No treatment hinges on getting an early test result, and the things that people do are probably a good idea whether you have the abnormal gene or not, or at least won’t hurt, such as exercising and eating right.” For children and teens, Dr. Nance says, the psychosocial repercussions of learning test results when there aren’t symptoms can be huge. “The parent who tests his asymptomatic 10-year-old because of guilt, concern, or a desire to plan, removes that child’s freedom to choose. There’s a 90% chance that child, if able to decide for himself, wouldn’t want to be tested.”
Another problem is that it can be very hard to tell when symptoms start, and if they indicate HD or something else. Does a teen who can no longer multi-task at a restaurant job have the family legacy? Is anxiety or irritability due to HD?
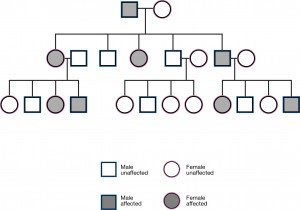 The multi-generational nature of the disease complicates matters. “We’re hesitant to diagnose HD in a 13-year-old from a challenging home environment, usually an affected father who probably isn’t working and may have bizarre behavior. The last thing we want to do is take a kid who is profoundly depressed or acting out, whose father is dying of HD, and do a gene test that shows he has a mutation of a size that generally causes symptom onset in a person’s 40s. Then we have just done a predictive test in an unstable 13-year-old,” Dr. Nance explains.
The multi-generational nature of the disease complicates matters. “We’re hesitant to diagnose HD in a 13-year-old from a challenging home environment, usually an affected father who probably isn’t working and may have bizarre behavior. The last thing we want to do is take a kid who is profoundly depressed or acting out, whose father is dying of HD, and do a gene test that shows he has a mutation of a size that generally causes symptom onset in a person’s 40s. Then we have just done a predictive test in an unstable 13-year-old,” Dr. Nance explains.
Very few physicians are trained to recognize JHD. Specialists in movement disorders work with older adults, such as those with Parkinson’s disease, and pediatricians rarely encounter HD. “So a child with HD symptoms will either be seen by a pediatric neurologist who knows little about HD, or by an HD neurologist who knows little about kids,” Dr. Nance says.
Diagnosis typically takes 2-7 years as physicians await obvious motor symptoms, or a clear decline in cognitive function. This is too long for families to wait. Dr. Nance and others are working to find better tools to determine when a child’s challenging behavior is just “being a teenager” or some other problem, and when it is due to the onset of HD.
MY CONNECTION TO HD
My family doesn’t have HD, but the disease has woven in and out of my life. Marjorie and Arlo Guthrie encouraged me to pursue science writing after reading a newspaper article I’d written in 1978. It was about my visit to Dr. Michael Conneally’s medical school genetics class at Indiana University, which featured 16-year-old twins with JHD.
Then in 1983, on a muggy May evening, I got a call from Peggy Wallace, who’d taken my human genetics course at Miami University and gone on to do her PhD with Dr. Conneally. His lab was one of four seeking a genetic marker for HD.
Peggy was the first to realize they’d found a marker. Peggy – Dr. Margaret Wallace – went on to post-doc with Francis Collins and then to discover several disease-causing genes, at the University of Florida.
I pitched the HD marker story to popular magazines, but none were interested in such a rare disease. Instead, in those days before the human genome project was even a dream, I wrote about the marker in a wonderful but extinct magazine called High Technology, and in Issues in Science and Technology. I did some preliminary research to write a book about finding the marker, but got little cooperation from the researchers. Alice Wexler, whose mother had HD, eventually did a far better job than I could have.
It took a decade for researchers to finally find the HD gene, a journey complicated by the gene’s location out on the tip of chromosome 4. By 1994 reliable genetic testing for HD became possible for anyone – the older marker test would only work if the indirect DNA sequence could be followed in several family members.
The third chapter in my HD story was Ray. Because of all of the above, when I applied to be a hospice volunteer, I requested an HD patient – something highly unusual, for most hospice patients have cancer.
Ray, then 44, was the last of several siblings who had HD. He’d lived so long with the disease that his worn-out body had ceased the relentless movements. He was eerily still, able to communicate only with his eyes. But the staff at the nursing home, who’d cared for Ray’s older siblings, now gone, and for Ray for 8 years, told me that he loved rock music.
I shared the last four months of Ray’s life, in spring 2005. I communicated with him via a shared iPod, inventing my own music therapy, and wrote a semi-true novel about the experience.
By the end, Ray was skeletal, curled into himself, his organs having shifted in his deformed body in the same way that Jane told me her little girl had become twisted. On the day before Ray died, I wondered why he wouldn’t shut his eyes, as cancer patients do, so I called Dr. Conneally in Indianapolis. He remembered me. “Ricki,” he said quietly, “he won’t close his eyes because he can’t.”
Today I sometimes write for the CHDI Foundation (Cure Huntington’s Disease Initiative), “a global private foundation funding HD science” to the tune of $100 million or so last year. CHDI holds 2-day workshops in which they throw a dozen researchers connected by a general theme – lipid biochemistry, rating scales, stem cells – into a room, and someone like me produces a report summarizing their brainstorming. A CHDI gig is a coveted assignment — always an opportunity to learn.
THE CHALLENGE OF CONQUERING HD
CHDI, HDSA, and others fund an enormous amount of research into developing treatments for HD, from cell biology to population studies that track the disease’s unfolding.
But I’m concerned. The quest that I learned about from Marjorie Guthrie in the 1970s has been going on for too long, the goal too elusive, because the triplet repeat diseases are so unlike other inherited ills. They can’t be fixed by replacing an enzyme or countering a biochemical buildup with diet, or by sending in a normal-length gene, for there’s already one there. The HD mutation is of the nefarious “gain of function” variety. Even refolding the errant protein, as has worked so beautifully in treating cystic fibrosis, hasn’t happened. Silencing the extra CAGs may be the way to go; antisense, RNAi, and zinc finger nuclease approaches may work.
 Basic research must keep the drug candidates coming, but support should also focus on the daily challenges that people like Jane Mervar face so gallantly. Jane and her girls have done much for the HD and rare disease communities by sharing their story, which I’ve only touched on here. Even if a gene therapy or repurposed drug or nutritional supplement is never found, there’s still much that health professionals can do to help families with HD. Jane explains how:
Basic research must keep the drug candidates coming, but support should also focus on the daily challenges that people like Jane Mervar face so gallantly. Jane and her girls have done much for the HD and rare disease communities by sharing their story, which I’ve only touched on here. Even if a gene therapy or repurposed drug or nutritional supplement is never found, there’s still much that health professionals can do to help families with HD. Jane explains how:
“The docs I respect and trust the most are those who can explain what is occurring, and if they cannot help they seek the person who knows the best answer … Teams of specialists helped me keep Karli at home until the end. The last 6 months were the most difficult, meeting her spirit and comfort needs. But she passed on her terms, and I knew we gave it our all.”
May is Huntington’s Disease Awareness month. To help the young people who have this cruel mutation, please contact the University of Iowa HDSA Center of Excellence for Juvenile Huntington’s Disease, where Jane Paulsen, PhD, heads up the JHD effort. One hundred percent of donations fund the research.



Ricki, this is a wonderful piece of writing, and so informative. Great job!! I intend to assign this to our genetics freshman.
Thanks! Where do you teach? Credit goes to Jane for sharing her story.
UW-Madison
[…] Juvenile Huntington's Disease: The Cruel Mutation Instead, in those days before the human genome project was even a dream, I wrote about the marker in a wonderful but extinct magazine called High Technology, and in Issues in Science and Technology. I did some preliminary research to write a book about … Read more on PLoS Blogs (blog) […]
Continuing to pray for Jane and her family. In God we trust.
Mixing the treatment with the alternate system of medicine may help in giving some comfort , my wife suffering from the Huntington,s was having problem to swallow the food ,by adding few medicine from the Ayurveda and homoeopathy have helped in improving the condition also in improving the speeach
Yes there are things that can be done. A friend of mine found that niacin supplements helped his wife. Until there’s a mechanism-based treatment, handling symptoms to improve quality of life seems the way to go.
Excellent, Ricki! Very informative. I’ve known some people with the HD gene and what you have written here has added to what I learned from them.
[…] Juvenile Huntington's Disease: The Cruel Mutation Looking back, signs that Jane Mervar's husband, Karl, had Huntington's Disease (HD) started about when their youngest daughter, Karli, began to have trouble paying attention in school. Karl had become abusive, paranoid, and unemployable due to his … Read more on PLoS Blogs (blog) […]
Congrats to Chelsea!
I can relate to the fact that most neurodegenerative diseases are exceedingly
aggressive,when my husband used to have seixures he lost memory cells.
People with epilepsy,have serious difficulty with memory after a seizure,
because everytime they phase out or lose consciousness,they do not regain
the large portion of neurons,that played a part in their motor control that
was lost during the grandmal seizure,or the memory cells because their
arrousal timing is comprised of confusion and loss of timing.
Even certain brain tumors require unconventional treatment,such as
astrocytomasmultiform which are wrapped around other delicate parts of the
brain,that control cognitive function,movement,speech,vision and respiration
so the neurosurgeon has to seriously consider the risks versus the benefits of
removing that brain tumor or use an unconventional surgical tool to remove it.
Huntingtons Disease is a very complex polymorphic nucleotide
repeat disease, Despite that its a dominant familial disease,The neurobiologist,
has to find out where it started expanding within the pedigree and find a
molecule to stop its devastating growth.
Although,Amyotrophic lateral sclerosis,isn’t always a
hereditary disease,The ALS Association is reporting that,a mutation called
the Sulphur oxide dimutase one seems to be the culprit in causing the
highest percentage of ALS cases along with agent organge a pesticide that
war veterans were using to cloud the visual ability of other fighter pilots in
Vietnam,Guam,Korea,Pakistan,ect and mustard gases which were found to
have neurotoxic contents.
ALS Association is working on Gene therapy,they would like to be able to silence the aggressive SOD-1 mutation that is partly responsible for a large percentage of ALS occurences.
However,There is a neurobiologist at NorthWestern University,
Dr Teepu Sadique MD,who has been working on an Familial ALS mutation
so the cause for amyotrophic lateral sclerosis may have some mild
genetic similarities to Huntingtons Disease,just not alot.
Patients with ALS do not suffer from cognitive decline,nor do they
start screaming,get rowdy,or paranoid.
The ALS patient does share the potential for getting depressed and
wanting to give up towards the point when they will need a ventilator and
suction machine to them this is not a real existence.
Excellent article,Huntingtons Disease is a devastatingly aggressing disease,
I have known that neurological disorders were aggressive
for 40 years,I have friends and a spouse with epilepsy,and the seizures cause
permanant memory loss,brain cells die,they dont regenerate.
That is why patients with Glioblastomas and neuroblastomas have
very low survival rates,thses tumors are metatastic,they grow like weeds
and they wrap themselves around other delicate parts of the brain.
I come from a big medical family and I have gone to
college,so I go to the medical library at SouthSide Hospital in my local
Community when Iam off from work.
My cousin Ivan is a psychopharmacologist and he taught psychiatric
nursing at Columbia University,my father was a clinical psychotherapish
who worked with autistic/children on the Spectrum.Ivan’s father was
a pathologist a Weill Cornell New York Hospital. I Think the logical
plan would is to research wasys to modify the expansion of the nucleotide
chain growth.
If the cag nucleotide chains are multiplying at dangerous speeds
in which molecular mayhem is occurring,then there definitely has to be a
way to totally slow down the speed of this particular one that is causing so much genetic devastation.