Alani’s Life With Lipodystrophy
We tend to think of fat as the enemy when it bulges over our waistlines. But fats are essential to survival. We need cholesterol to make sex hormones, fatty acids to assemble into the membranes that wrap around our cells and form the organelles within, and lipid deposits beneath the skin and around organs to keep us warm and protect against starvation. Yet as in all matters biochemical, balance and distribution are critical.
When fat is abnormally deposited in the body, a lipodystrophy results. The person appears to be all muscle, a mirage of health. But on the inside, the fat molecules are building up where they shouldn’t, in the blood and in solid organs like the liver, heart, and other muscles.
Last month I met Rachel Daniels at the annual Breakthroughs Summit of the National Association for Rare Disorders (NORD), an organization for which she’s a patient advocate and Oklahoma State Ambassador. Here, she describes how she found out that her young daughter has a lipodystrophy.
RACHEL’S DIAGNOSTIC ODYSSEY
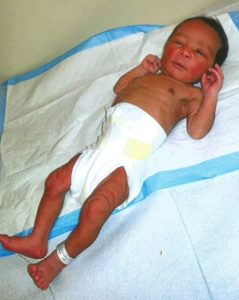 “Born in January 2014 was my sweet Alani. Just over 5 pounds, she was so small, but so beautiful. She had an awfully large belly to be so new, and I noticed that she had two hernias in locations that concerned me, but I was assured they would resolve on their own. Her head seemed large.
“Born in January 2014 was my sweet Alani. Just over 5 pounds, she was so small, but so beautiful. She had an awfully large belly to be so new, and I noticed that she had two hernias in locations that concerned me, but I was assured they would resolve on their own. Her head seemed large.
At birth Alani was extremely muscular. I mentioned her frail yet defined appearance.
“Be thankful to have a future gymnast on your hands,” reassured the doctor.
“But why is she so stiff?” I persisted.
“It’s part of the birthing process,” came the response. It was not normal, and I knew that, but I got pushback from doctors.
Discharge went as planned and I took Alani home. Still with lingering thoughts about her incredible physique, I typed “muscular babies” into Google. Image after image popped up of babies with legs and arms of a body builder. Captions mentioned “dystrophy”. I decided to search further.
Over the next couple of months, Alani flourished, and we watched her grow, although she was different in appearance from her siblings. I grew concerned about what was going on with her internally when she picked up an overwhelming desire to eat constantly, as though never full. I nursed her to the best of my ability and immediately had to substitute formula. After each bottle, she would cry for more until she received yet another. And another. And another.
Before we knew it, it was time for first shots. At the 3-month appointment, I sat holding Alani thinking how I would tell her pediatrician that I was refusing immunizations. She had a cold so I could use that. So I blurted out that we would be refusing shots. Shocked, the pediatrician asked what was wrong. Alani didn’t have a fever, so shots would be safe…. so I told him. Everything.
He asked what I wanted to do, so I said I wanted to go to the hospital. He immediately admitted us to Children’s Hospital at OU Medical Center in Oklahoma City, in April 2014. We stayed 3 days, presenting with a severe cold and concerns of extreme muscular appearance.
On the 1st day we were overwhelmed with questions as we detailed our concerns to all doctors and nursing staff that came into our room. The 2nd day a genetics team came in to look at Alani, and asked me what I thought she had. I told them it was some form of a dystrophy but I didn’t know what. They examined her and assured me they would be back.
Indeed they came back, with medical students and other staff, and I immediately felt faint. The genetics team felt she had a form of lipodystrophy, but without genetic testing they would be unable to tell us exactly what type. I began sobbing uncontrollably and nothing could console me. Appointment times and days were set to begin testing. Life as I knew it would never be the same.
In May 2014, we received confirmation that Alani has congenital generalized lipodystrophy. Her specific mutation is in the gene AGPAT2.”
 CONGENITAL GENERALIZED LIPODYSTROPHY
CONGENITAL GENERALIZED LIPODYSTROPHY
Alani’s disease is autosomal recessive, inherited from carrier parents. Other genes that cause CGL are BSCL2, CAV1, and PTRF. All four forms are autosomal recessive and affect the cells (adipocytes) that normally store fat. BSCL2 affects the brain and may cause intellectual disability. If children with CGL symptoms have normal versions of these four genes, it’s possible that they have a form for which the causative gene has not yet been identified.
RACHEL CONTINUES …
“Alani’s blood tests revealed extremely high triglycerides and her leptin levels were dangerously low, among other medical issues. She has no fat under her skin, but fat in the bloodstream, which ultimately can cause a host of medical issues. She can die of severe pancreatitis, a fatty liver, an enlarged heart, diabetes, or leptin deficiency in the brain.”
LEPTIN
The hormone leptin rose to fame in the mid-1990s, when in the wake of its discovery and ability to shrink obese mice, it briefly became a contender for a magical weight-loss pill.
Leptin is produced in fat cells and travels in the bloodstream to the brain, where it signals satiety. So increasing leptin levels should halt hunger– but it wasn’t so simple. Injections of leptin helped only the handful of people who can’t make the hormone. People with obesity actually have plenty of leptin – they just can’t respond to it, a little like the situation in type 2 diabetes.
Supplement companies still hawk leptin, but circuitously, because as a small protein leptin is broken down in the stomach. Here’s a buy-1-get-2-free offer for 11 types of leptin products from one company.
Leptin products range from the vague – “promoting leptin function” – to the vaguer – “addressing emotional eating” — and are concoctions (patented of course) of mostly fiber (lots of algae and seaweed), with a few vitamins like beta carotene thrown in. Many tablets also have green coffee bean extract, once the elixir-of-choice of the good Dr. Oz until he backed away from the claim. Caveat emptor.
But Alani needs actual leptin.
“I fell into an immediate state of depression.
Research began.
Countless doctor appointments came and went.
Alani was placed on a special formula called Enfaport by Enfamil. It maintained her triglycerides at safe levels, and was her main source of nutrition for the first year. But then nutritionists got involved because she wasn’t receiving the recommended daily nutrition and demanded that she be removed and fed an extremely restricted diet, because she had exceeded the recommended age for this formula. As a result of her delayed introduction to solids, she didn’t learn how to chew properly. Now at nearly 3 years of age, she still chokes on her food and has to have it chopped up finely.
Discouraged, I decided to start channeling outside sources for help. I spent so many sleepless nights networking, requesting information as well as sending pictures and information to doctors, professors, anyone who had heard of her condition.
Responses soon flooded my inbox!
Dr. Elif Oral, associate professor of endocrinology and internal medicine at the University of Michigan, sent for us! So our first adventure was to a lipodystrophy symposium in Ann Arbor, late that year. Then, a groundbreaking trip to NIH in Maryland, where I was trained on how to administer Alani’s Myalept injections.”
REAL LEPTIN
FDA approved Myalept (metreleptin for injection) on Feb. 24, 2014, to treat leptin deficiency, in patients with Alani’s condition as well as certain other inherited and acquired forms of generalized lipodystrophy. The drug is a chemical cousin of leptin manufactured using recombinant DNA technology. Aegerion Pharmaceuticals is beginning a safety registry to track any adverse effects. An acquired form of lipodystrophy affects people with AIDS, but that wasting develops slowly and is not an indication for Myalept.
 RACHEL CONTINUES …
RACHEL CONTINUES …
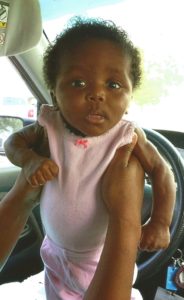
“Yes, it happened that fast. One minute I had no idea what was going on, the next minute I was dragging suitcases and packing my baby in my arms in airports to connecting flights to see doctors from around the world. It has been an incredible start to a journey I know will present endless opportunities, and I’m forever grateful to those who extend their hands out to us in love and friendship. We are spreading awareness for lipodystrophy through publications, media, and appearances at conferences, galas, and medical events throughout the US.
Alani is 1 in 10 million. The only treatment for her CGL is the daily injection to replace, stabilize, and maintain her leptin levels to prevent endocrine issues. Her insatiable appetite complicates daily life. She can’t have any food that has fat, and it must be fresh or frozen. No cake or cookies, and just 1% milk and water. That’s 525 calories a day! The inability to feel full is a fear no mother wants for her child.
People often ask what I expect of Alani. Well, I expect for her to be a world class Olympian, a gold medal gymnast, and president of the world. I expect what any mother would of her child: only the best. But all I have is hope. Hope that she’ll beat the odds against her. Hope that we’ll beat lipodystrophy … together.”
To Help:
Lipodystrophy United
NORD
Global Genes
EveryLife Foundation for Rare Diseases
Please contact me if you’d like me to cover a specific rare disease.