Don’t Tell Me My DCIS Isn’t Cancer!
“DCIS isn’t really cancer. You have nothing to worry about,” said my oncologist confidently.
“Then why am I having a mastectomy in four days?” I blurted.
“DCIS doesn’t spread. So it isn’t cancer.”
“But the “c” stands for carcinoma, a cancer of epithelial tissue. How is that not cancer?” I asked.
“DCIS. Can’t. Spread.”
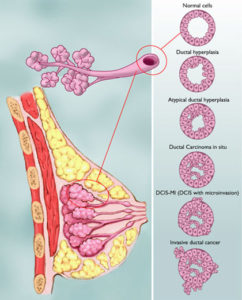
Case closed. But I knew what he meant. Ductal carcinoma in situ isn’t cancer, some say, because “in situ” means “in place,” and invading healthy tissue is one of the nine characteristics of cancer I’ve listed for years in my textbooks. Eight out of nine was enough to convince me that Hannibal had to go.
Why name my DCIS?
 If Hannibal Lecter, the fictitious cannibal serial killer in the book and film The Silence of the Lambs, remained in prison, he couldn’t eat any more people. But if he got out, he could. Does that mean that the incarcerated Hannibal isn’t a cannibal, just because he’s temporarily contained? Of course not. Likewise, the risk that the abnormal cells that filled a duct in my breast would spill out and spread into an invasive cancer, if not removed, was about 40 percent, likely within 5 years.
If Hannibal Lecter, the fictitious cannibal serial killer in the book and film The Silence of the Lambs, remained in prison, he couldn’t eat any more people. But if he got out, he could. Does that mean that the incarcerated Hannibal isn’t a cannibal, just because he’s temporarily contained? Of course not. Likewise, the risk that the abnormal cells that filled a duct in my breast would spill out and spread into an invasive cancer, if not removed, was about 40 percent, likely within 5 years.
Confusing Terminology
DCIS is considered stage 0, but it becomes stage 1 (DCIS with microinvasion) when it breaks through the milk duct wall. Once through, it’s invasive ductal carcinoma (IDC). But that’s not all.
“Grade” describes the shape that the errant cells pile into, which reflects their division rate – papillary (finger-like), cribriform (like Swiss cheese), or solid, for low grade (I) or moderate grade (II).
But if the grade is high (III), like mine, the duct is filled and has dark spots (called comedo necrosis) where the cells are dividing so fast that some of them starve to death. Wonderful. Gene expression patterns and hormone receptor status further describe DCIS cells.
 I knew my doctor meant well, but I’d seen the mammogram and read the biopsy report and knew Hannibal was on the brink of escape. The oncologist evoked an oxymoron: If DCIS escapes the duct, it’s no longer DCIS, but IDC. Therefore, DCIS can’t be cancer. Hannibal can’t be a cannibal.
I knew my doctor meant well, but I’d seen the mammogram and read the biopsy report and knew Hannibal was on the brink of escape. The oncologist evoked an oxymoron: If DCIS escapes the duct, it’s no longer DCIS, but IDC. Therefore, DCIS can’t be cancer. Hannibal can’t be a cannibal.
I didn’t think much more about the doctor’s downplaying until I saw a post on a closed Facebook group I’m on with about 15,000 women at various stages of the breast cancer journey. A woman’s husband was refusing to take time off work to help her in the days following her surgery because “the doctor said it isn’t really cancer.”
That’s a game changer.
Medical students are asked to recite “primum non nocere,” or “first, do no harm,” which comes from ancient Greek physician Hippocrates’ Of The Epidemics. Saying cancer isn’t cancer to calm fears can indeed do harm.
Patients Speak Out
When my PLOS editor asked bloggers to post about cancer this week, to coincide with the American Association of Cancer Research (AACR) annual meeting, I thought I’d ask the breast cancer group about DCIS being “not really cancer.”
Within minutes, several versions of “If DCIS isn’t cancer, why a lumpectomy or mastectomy?” appeared. Not a single woman considered her DCIS anything but cancer.
“Calling DCIS not cancer made the journey so much harder for me. It took me 5 months to figure out what to do … 5 months of sleepless nights, stressed days, and constant thinking. I have found it all quite traumatic.”
“In my opinion DCIS is definitely cancer and it is not helpful to suggest otherwise. It is not YET invasive, but has the ability to become so. It is defined by its histological features, and those features involve the characteristics of cancer cells.”
 “I never really thought about this before, so I searched it a bit. The first thing this article lists about DCIS is that it’s NOT cancer because cancer has to be able to grow and spread unabated. I think saying that it is not cancer because it has not YET spread is very misleading.”
“I never really thought about this before, so I searched it a bit. The first thing this article lists about DCIS is that it’s NOT cancer because cancer has to be able to grow and spread unabated. I think saying that it is not cancer because it has not YET spread is very misleading.”
“The medical world is not in agreement on this at all. If they aren’t clear about it, then how could the patients be?”
Having cancer is terrifying enough, without having to interpret mixed messages.
Active Surveillance for DCIS?
A few women’s doctors mentioned not treating DCIS and just seeing what happened – but no one chose this option.
“I’m not about to sit around waiting to see if this thing breaks out and invades other areas or not. No, thank you. When the doctor told me about a study to leave it alone, I did not jump up and ask “oh, how do I get into that study?” I realize that I am taking a big chance that this treatment is not necessary, but I’m not willing to bet any other way,” wrote one woman.
She’s right. There’s already plenty of evidence that even a low-grade DCIS allowed to sit around in situ may eventually burst its boundaries. Here’s an article that helpfully puts its conclusions in the title: “Continued observation of the natural history of low-grade ductal carcinoma in situ reaffirms proclivity for local recurrence even after more than 30 years of follow-up.”
Still not cancer?
An ongoing 84-center clinical trial is conducting the obvious experiment: comparing the fate of women who have low-grade DCIS with and without surgery. The untreated participants do active surveillance, similar to what’s been done for prostate cancer for more than a decade. Active surveillance requires more frequent diagnostic testing than simply “watchful waiting.”
Economics seems to be driving the study, not necessarily the angst that we women feel when bad news is dumbed down. “The national health care expenditure resulting from false positive mammograms and breast cancer overdiagnosis has been estimated to approach $4 billion annually. There is general consensus that much of this burden derives from the treatment of DCIS; for those estimated 40,000 women per year whose DCIS may never have progressed even without treatment, medical intervention can only harm,” states the ClinicalTrials.gov listing.
The study is following 1200 women for 2 years, 600 having undergone lumpectomy or mastectomy and 600 not, to see how many develop IDC on the same side as the DCIS. The cancer cells must be estrogen or progesterone receptor positive, the tumor grade I or II, and no comedo necrosis.
 It’s a terrific experimental design because the secondary outcomes assess repercussions of having breast cancer that I didn’t even know existed until it hit me a few months ago. The study is probing the obvious – risk perception, anxiety, depression, and body image – but also “intolerance of uncertainty” and “decisional regret.” It also is examining “communication with physicians” (hello?) and employment and financial status, two huge sources of stress. Descriptors for “specific breast pains” in the analysis are wide-ranging, from the chronic and serious post-mastectomy pain syndrome to what I call ETZs (electric titty zaps).
It’s a terrific experimental design because the secondary outcomes assess repercussions of having breast cancer that I didn’t even know existed until it hit me a few months ago. The study is probing the obvious – risk perception, anxiety, depression, and body image – but also “intolerance of uncertainty” and “decisional regret.” It also is examining “communication with physicians” (hello?) and employment and financial status, two huge sources of stress. Descriptors for “specific breast pains” in the analysis are wide-ranging, from the chronic and serious post-mastectomy pain syndrome to what I call ETZs (electric titty zaps).
Another measure is “concerns about future breast events.” That’s huge. Once a woman is deemed “NED” (“no evidence of disease”), is it better to be an ostrich, or read every new study? And should I consider population studies or anecdotes?
Good News
Statistics say the chance of IDC following DCIS surgery is less than 1%. But Facebook posts of cancer’s return aren’t unusual: “I was diagnosed with DCIS in 2007. No chemo or radiation. Lymph nodes clear. Mastectomy out of fear and took Arimedix for 5 years. In 2016 it came back in my spine and 2 spots in my lungs.” I’ve been informally keeping track and 9 years seems to be a common point of return. So much for the olden days when a cancer was considered “cured” after 5 years had passed. NED, not cure.
I was cheered to find media coverage of a study from about a year ago, “Women With DCIS Live Longer Than General Population.” The study, actually a poster presented at the 2017 European Cancer Congress, tracked 9,799 women treated for DCIS in the Netherlands from 1989 to 2004 for 10 years. About 3% of them died from breast cancer, only slightly more than the general population. But the women were less likely to die from a bunch of other conditions, because, the researchers conjecture, they’re more health-conscious than most folks.
 Alas, a quote from the researcher clouded my joy. “There are a lot of uncertainties and anxiety associated with DCIS because many patients think they are diagnosed with breast cancer. Some DCIS lesions will progress into invasive breast cancer and can metastasize and then cause death. So it’s important to look at the outcomes,” said Lotte Elshof, of the Netherlands Cancer Institute in Amsterdam. Did I just THINK I was diagnosed? What was the biopsy then, a random boob harpoon?
Alas, a quote from the researcher clouded my joy. “There are a lot of uncertainties and anxiety associated with DCIS because many patients think they are diagnosed with breast cancer. Some DCIS lesions will progress into invasive breast cancer and can metastasize and then cause death. So it’s important to look at the outcomes,” said Lotte Elshof, of the Netherlands Cancer Institute in Amsterdam. Did I just THINK I was diagnosed? What was the biopsy then, a random boob harpoon?
Another way to use new findings is to more finely parse the diagnosis: “Women with DCIS at lowest risk of recurrence if they are post-menopausal or ER+,” claimed one recent study. Such population trends are interesting, but I wanted genetic evidence – and those findings aren’t so good.
Bad News
In a study published in Cell in January, researchers sequenced the cancer-causing mutations in 1,293 tumor cells from 10 patients, comparing the genetic profiles of DCIS cells to those of IDC cells in the same woman. A Nature News and Views about the report notes “the remarkable genetic similarity of a patient’s tumour cells in these two distinct disease states.” That is, the mutational seeds of invasiveness are right there in DCIS.
Still not cancer?
I’m hopeful that ongoing investigations of gene expression and epigenetic patterns may find a way to predict which DCIS cells will go rogue.
A paper in this week’s Science Translational Medicine also caught my attention, if so far applicable only to rodents. Robert Weinberg of the Whitehead Institute and colleagues found that T cells in uninjured mice could attack injected cancer cells, but tumor cells injected into mice healing from an injury metastasized. Might surgery to remove cancer divert the immune system into healing, allowing bits of dormant cancer elsewhere to spring up? “The new study may explain why breast cancer metastases sometimes appear 12 to 18 months after surgical intervention, an outstanding question that has long been debated,” announced the news release. Happily, though, anti-inflammatories kept the mouse tumors small.
Final Thoughts
I’m not content with my oncologist’s “DCIS isn’t really cancer.” Genetically, it is. Histologically, it is. And the pathology report indicated that even though the margins around the filled duct were clear, Hannibal was sliced but not diced – only “representative sections” submitted for analysis. That leaves room for the ticking time bomb that is cancer.
A breast cancer diagnosis divides time. In the after, my new normal, I think often, too often, of that ticking time bomb, although I know the statistics say it isn’t likely to detonate. So I’ve decided to acknowledge my fear for just a moment every morning. And then get on with appreciating the new day.
Other DNA Science posts about breast cancer:
Rare Disease Week Through a New Lens: Having a Common Disease, Breast Cancer
How Genetic Testing Guided My Breast Cancer Journey – to Eschewing Beef
Dueling BRCA Databases: What About the Patient?
Assessing Breast Cancer Risk: Beyond the Angelina Effect


Thanks for your insight, i am going through the same ” its not cancer” situation with a pancreatic cyst, even though every one of my doctors says its the exact kind that turns into cancer, and they will not take it out, at all, until it is cancer, that sound like shutting the door after the chickens have flown the coop. Im asknazi jew , with astronomical cancer risks, and docs dont seem concerned , they think watching and waiting is the only option.
Hi Sherri. Often a cyst will just collapse and go away — that happens in the ovary. It is just a fluid-filled sac, with none of those characteristics of cancer I listed. But a cyst (or polyp in the colon) can mask a cancer underneath it. I hope it all works out for you!
[…] Source: Don’t Tell Me My DCIS Isn’t Cancer! […]
Wow…that was me diagnosed with highgrade dcis 12/2017 i’ve been agonizing on what do to….my surgery is scheduled for 5/3/18…
You should have surgery, to get rid of it and peace of mind. And join Breast Cancer Straight Talk on FB, I don’t know how I would have gotten through this without the group. You and I are lucky though, it is early stage. Email me through my website (www.rickilewis.com) to chat more if you like. I’m not an MD but being through this teaches you a lot. You will be fine and feel much better once it’s over! Thanks for writing.
Hi, thank you for this article. I am going through this exact thing, it has all happened so fast and I’m getting a second opinion next week but def planning surgery. I appreciate your candor and the information. I will check out your site.
Oh my God! My brother-in-law, a practicing gp of 29 years, has been touting around my family that my high-grade DCIS and the resulting mastectomy was not breast cancer. I can’t tell you where I am in my mind…. help!
Sometimes physicians do not know, or have forgotten, biology. The C in DCIS is “carcinoma,” and that is a cancer of epithelial cells. Some people do not consider DCIS a cancer because it has not spread beyond the duct. But I sure wasn’t going to leave it alone and wait for it to do so!
I am so sorry that you have been through this too. x
I was diagnosed with DCIS in October 2020 & has several biopsies taken in November. Following my results that most of the calcifications has actually been removed during the biopsies, my cancer specialist was happy to just monitor my yearly screenings, on the condition that if they had multiplied I would opt for lumpectomy if appropriate. After reading everyone’s treatments I am wondering if I made the right decision. My husband & family think it is not serious as it was called pre cancer.
DCIS isn’t pre-cancer because the C stands for carcinoma, which is an epithelial cancer. But it sounds like your biopsies may have removed the suspicious cells! This happened to my best friend. Doctors have a way of softening alarming news – beware “pre-cancer” if carcinoma is part of the name, “lesion,” “scar tissue,” “cure,” and especially “cancer-free.” We do not have the technology to tell if someone is cancer-free, that would entail examining every cell! Doctors mean well, but the softening can be misleading.
Hi. Thank you so much for sharing this. I am exactly in the same situation. It is just that I already got surgery, got rid of all of my left breast saving the nipple. My doctor prescribed me to take Tamoxifen for five years along with 20 sessions of radiation therapy. I’m on the medication. However, I gave up on radiation therapy after the fourth session. I cried with Mom, and she told me that she would die with me if cancer comes back and that we will put off the radiation therapy until then. Recovering from the surgery was hard, but radiation therapy was killing me with nausea and destruction of my immune system. I am still worrying over my decision to skip radiation therapy. Then, I encountered your post. Did you get the radiation therapy?
No I didn’t get radiation. I would have if I’d had a lumpectomy, but I opted for the mastectomy. Good luck and stay well!
I also did a mastectomy, but then the doctor said that my cancer was very close to the skin. So, radiation can kill all the possible residues. However, after the fourth therapy, I gave up. I could not function anymore. My lips got all peeled off. I had fibers filling up underneath my breast. It was itchy underneath the skin because radiation burned the inner skin tissues that they started its healing process. So… hospitals kept on calling me, but my mom and I cried that we will just die together if it happens again…And… I’ve been taking Tamoxifen every other day after reading journal articles about the experiment that was done in Italy.
My feeling is that not even doctors do not know with certainty. That makes me confused and lost all alone in my mind. So… how are you getting along?
No one can ever know if a cancer is truly, permanently, gone. That is why I dislike “cancer-free.” Take things one day at a time. It sounds like you’ve done so much! Enjoy life.
I’ve just been told my pathology report after my mastectomy – 77mm DCIS with no spread to lymph nodes (7 removed.)Medium and high grade. I should be juvulant but I’m devastated. Biopsy had suggested underlying invasive cancer. But if it’s just DCIS then why have I lost my breast??? Lost, confused, and wishing I was dead.
Lara, how long has it been since you’ve been treated? I found that the intense emotions do fade with time. 77 mm is fairly large, so I think you and your docs made the right decision (but I’m not an MD). The emotions may depend somewhat on your age – less devastating if you’re much older. No spread to lymph nodes is the best news you could get!
Hi it’s Lara again- sorry I only just noticed your reply. My mastectomy was 4th May so I’d written that comment quite soon after. I’m feeling better now but still annoyed when the word pre-cancer was used at my recent appointment. It’s pre-invasive, but correspondence from the doctors have mentioned cancerous cells. I may write to them to ask them to change their terminology cos I wouldn’t have let them have my breast unless it was cancer, and l don’t want other women to go through the hell I went through.Thank you for your article and your support- it has really made me see things clearly.
Yes, pre-invasive! Glad you are well!
Imho, in order to be more balanced, please discuss the frequent re-excisions and lymphodema risks that are associated with Standard of Care treatments, the side effects of radiation. There are women in the Facebook groups that have been severely affected by treatments. I don’t know how you can be definitive about DCIS being cancer when there are experts that say a mutation is needed to become invasive. We have the option of choosing lifestyle changes. Researchers agree that intermittent fasting and exercise have been shown to decrease risk by 30% each.
Thanks. Those suggested topics are best addressed by an MD. We’re really just quibbling over terminology. If DCIS isn’t cancer, why does the C stand or carcinoma? Meaning cancer of an epithelial tissue. But since I wrote that article, DCIS that is exiting the duct has been described, so my article is a bit dated.
It it wrongly named – that is the issue. It should be called DAIS (ductal atypica in situ). Carcinoma in situ is a misnomer. A defining aspect of cancer is invasion. DCIS does is incapable of invasion. Yes, it could become invasive after a 2nd hit mutation, but the second hit may never occur. Your Hanabal analogous is not correct. Also “recurrence” often confuses women. They don’t understand that the whole specimen is not looked at, only a few slices. An invasive cancer may be present in the removed tissue but not picked up by the pathologist in the random slicing. So years down the line when a metastatic tumour presents, the woman thinks the DCIS she had removed years ago, has become “invasive” but the invasive cancer was there all along, but not picked up by the random slicing.ps I work in cancer research.
Thanks, excellent points.
Thank you for this – yours is the most succinct thing I’ve read. My brain has struggled with the ‘0 stage label’ – if it was zero it would nothing and why am I having surgery and radiation for a nothing?
My primary Dr and also my surgeon described it as the best bad scenario – this little f**cker called DCIS (thats how I refer to it-mine is high grade and all the other not great pathology words). Surgery is on Thursday -lumpectomy and then eventually radiation.
I also tapped my research scientist friends who will tell you all about cells and how they “stop communicating” properly – was helpful to understand how this shit happens. I am going to check out the FB group.
Hello.
Thank you for your article.
I was diagnosed with an intermediate dcis in March.
I have opted to have mine monitored.
It’s only 7mm in size and I’m negative on the gene test. I have also had two biopsies. The first done with the guidance of the scan and the second by touch. The second came back completely clear so the lump I feel is no indication on how larch the dcis is.
For me I feel it’s not necessary to have surgery.
I’m going to have a yearly mammogram to keep checking for any changes.
I understand how others have opted for surgery. I did to begin with. My family don’t agree with my choice and again I understand where they’re coming from.
That makes sense to me. I’ve often thought about this. I was able to see my mammogram right away because I do genetic counseling at the doc’s office, and I could see my tumor blobbing out of the duct! That made up my mind. Good luck to you!
July 2022 I had a breast biopsy and the next day was told it was IDC. However I had another spot they couldn’t biopsy at that hospital and was sent elsewhere.My breast surgeon called me with that result. I still remember every word he said, “Good news, it’s pre-cancer”. The first one was grade 3, HER2+, and 8mm in size. The second tumor was also grade 2&3 and 6mm. Surely it was about to BUST OUT OF THE DUCT (I.e. faster growing/HER2+). Six months later It still frustrates me that he said it was precancerous.
I originally wanted a mastectomy with immediate reconstruction but breast surgeon said it would take months to schedule both surgeons the same day. He suggested lumpectomy with sentinel node dissection and porta-cath placement. He said he wanted to get the “hard stuff” (chemotherapy) going and over first. I never wanted radiation because I was having a mastectomy (at some point)…. When I returned to my breast surgeon he tried to tell me that my prognosis wouldn’t be any better if I had the mastectomy. In other words, he wanted me to reconsider my original plan…. again. As a nurse, statistically he is right, but it wasn’t about numbers. For me, it’s a piece of mind. In 2022, I has 2 breast tumors, 2 polyps from colonoscopy, a large precancerous polyp in uterus and a grade 3 mole that’s path report states is a fine line between precancerous and melanoma ( or so my dermatologist says). I have heard enough of precancerous pathologies. Please don’t get me wrong, I am grateful everything could be removed, but IDC and DCIS are both cancers. Furthermore, they were mm apart.
However, I have now completed lumpectomy and chemotherapy. I took a new position at work and they have waited for me to finish chemo, so I am postponing the mastectomy and reconstruction until 4-5 mons after radiation (per plastic surgeon). I start radiation next week and I’m feeling stronger each day.
I will continue Herceptin every 3wks for 9mos and start anti-hormone pill after radiation. I have a treatment plan and am going to do everything I can to prevent a recurrence. Doctors are people too. They say the wrong things at the wrong time too. However, if they would stop teaching that DCIS isn’t cancer and change the name to “ductal carcinoma in situ breast cancer stage 0” it would make me happy at
By the way, I loved the article “Don’t tell me my DCIS isn’t cancer!” Well written!
Thanks Belisa. I’m glad that you know exactly what your situation is and that you have treatment options. I never regretted for a second having both breasts removed. I think if I didn’t I’d always be worried about recurrence. I hope you are well!!!
Hi, thank you for your article. I thought I was late to share but noticed you are still replying to comments. I was diagnosed with DCIS, 3 mm, grades low and intermediate, with one of the margins close, but still considered clear, ER and PR 100% positive, and a bit of necrosis, according to my oncologist.
On May 4th this year I had an excisional biopsy (afterwards called a lumpectomy) for my right breast so they could remove some atypical cells, and then those were sent to pathology. I get a call from my breast surgeon a week later saying that I have DCIS. I did not know what DCIS was at the time and said that is good news, right? And she said yes, it’s small, but you have breast cancer. She never said pre cancer.
I have a strong family history of breast cancer. Both my mom and younger sister died from breast cancer in their 50’s so I am choosing a double mastectomy with reconstruction. I was 38 when my mom died, and my sister died two years ago. I have done all my research, even the genetic testing which did come back negative. The thing is, my genetic counselor showed me the chart of percentages, and the BRCA1 and 2 genes account for 10% of all breast cancers, and familial history accounts for 20%. If I am doing the math right, I am actually at a higher risk than if I had the gene.
I am an active 62-year-old woman, and feel for my lifestyle that this is the best option for me going forward. I realize it’s a big surgery, but I certainly don’t want to be closely monitored and just see what happens. I was told I would not need radiation with a DM. I declined the hormone therapy because there are side effects and I don’t want to develop osteoporosis, high blood pressure, high cholesterol, hot flashes and some other menopause symptoms that I already went through, and joint stiffness. That would adversely affect the quality of my life. If I were younger, I would have possibly made a different choice.
Hi Teri, your situation is remarkably like mine. Yes, family history is very important, and a few dozen genes can cause breast cancer. I had a double mastectomy because I would not undergo chemo or radiation, and I didn’t want to have enough tissue left that I’d be constantly worrying about cancer returning. I am very happy with my decision – but a crazy way to permanently lose 8 pounds! Good luck to you!
Hi, I get so annoyed when I hear doctors and specialists say DCIS is not cancer and on that basis you will have no recurrence.
I was diagnosed in 2016 with multifocal DCIS leaving no question my only option was a mastectomy and removal of the sentinel node. The pathology was high grade with comedo necrosis, ER and PR positive the other was intermediate ER positive and PR negative.
Two years later my sister was diagnosed with the DCIS same side, multifocal and same outcome. Having a strong family history of cancer I had genetic BCNA testing which came back inconclusive. From all I have read and researched, a high grade result with comedo necrosis does increase the chances of early recurrence in the body.
I am at the 7 year mark and my recent ultrasound on the chest wall and mastectomy scar has shown an abnormality in the chest wall. I am booked in for biopsy next week. One would wonder if doctors believe DCIS is not cancer why do they subscribe to the radical treatments, regular mammograms/ultrasounds, lymph gland removal and biopsies on suspicious areas.
Thanks for this article. Every woman has a different perception of risk. I elected to do nothing for my intermediate grade DCIS which is against current “standard of care” especially as I’m only 47.
I feel for all women dealing with this diagnosis. It’s a pity that all of this cancer screening hasn’t moved the needle in overall mortality. Like an evil game of whack-a-mole. God bless to you all, and to the author, keep writing!
Thank you! I often wonder if I overtreated my cancer. But I did see it sneaking out of the duct on the mammogram.