Clues to combatting a devastating disease can come from identifying people who have gene variants – mutations – that protect them, by…
A Glimpse at a Future Heart Disease Drug Thanks to Gene Silencing
I often marvel at the disconnect between media coverage of “breakthrough” treatments and the decades of research that lie behind them. A new drug is the culmination of basic research, preclinical experiments on animals and cells, three phases of clinical trials, and post-marketing surveillance. It takes decades.
A small, phase 1 study – safety in healthy people – caught my attention this week. The work was presented at the American College of Cardiology’s annual meeting and published online in the Journal of the American Medical Association.
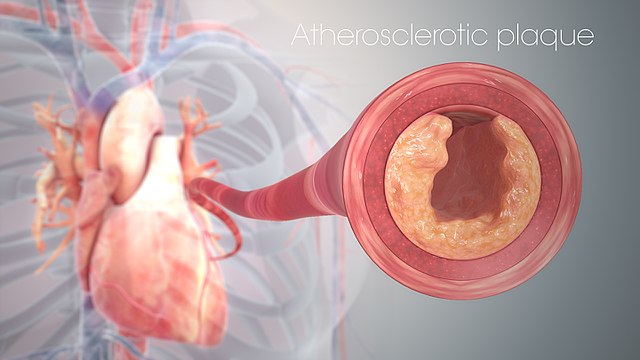
The healthy participants had elevated levels of apolipoprotein(a), which is made in the liver and goes to the blood, where it carries cholesterol. High levels raise risk of heart attack, stroke, and narrowing of the aorta. Could silencing the gene that encodes the protein portion of apolipoprotein(a) lower the level, perhaps even preventing the heart disease?
One way to silence a gene uses a natural process, RNA interference (RNAi), which blocks translation of a gene’s information into construction of a specific protein. The first drug using RNAi was Onpattro, approved in 2018 to treat a rare form of amyloidosis. The disease causes tingling, tickling, and burning sensations and affects about 3,000 people in the US.
In the new study, the researchers injected tiny pieces of short interfering RNAs (siRNAs), which glommed onto the messenger RNAs for the protein part of apolipoprotein(a). The 32 healthy volunteers received placebo or ascending doses. Levels of apolipoprotein(a) fell in a dose-dependent manner, by about 98 percent for the highest-dose group. All doses were well tolerated and the lowering largely persisted when checked at five months.
“These results showed the safety and strong efficacy of this experimental treatment at reducing levels of apolipoprotein(a), a common, but previously untreatable, genetically-determined risk factor that leads to premature heart attack, stroke and aortic stenosis,” said lead author Steven E. Nissen, MD, of the Cleveland Clinic. Future studies will follow clinical outcomes of the intervention.
A treatment to lower apolipoprotein(a) would be especially valuable because high levels are under genetic control. Lifestyle changes such as diet or exercise have no effect, as they do in lowering cholesterol.
A Brief History of Cholesterol Consciousness
Speaking of lowering cholesterol, a timeline of development of the statin drugs illustrates the incremental and small role of any one study, like the one just published on apolipoprotein(a).
1784 Identification of cholesterol in gallstones
1888 Four-ring molecular structure of cholesterol discovered
1910 First link of elevated cholesterol to atherosclerotic plaques
1913 Cholesterol fed to rabbits blocks their aortas
Until 1940, elevated cholesterol was considered an inevitability of aging. Diet and exercise components were not yet appreciated.
1939 Familial hypercholesterolemia linked to a mutation – homozygotes die in childhood, heterozygotes develop severe heart disease in early adulthood. Studying these patients led to development of statins.
1950 Epidemiological investigations reveal that HDL is protective
1960s Research ramps up:
• Biosynthetic pathway for cholesterol has 30 steps
• The third step is rate-limiting. Targeting HMG-CoA reductase will lead to first statin, mevalonate
• Framingham Heart Study strengthens link between elevated LDL and heart disease
1985 Michael Brown and Joseph Goldstein win Nobel prize for deciphering the regulation of cholesterol metabolism
1987 FDA approves the first statin, Lovastatin. It is now off patent.
2022 About 200 million people globally take statins. The U.S. market size is about $15 billion. With a GoodRx coupon, lovastatin costs as low as $1.50 a month.
The New Alzheimer’s Drug Controversy
I’ll end with a look at the newly-but-perhaps-prematurely-approved Alzheimer’s drug Aduhelm, which costs $28,200 a year. I can understand that price for a new cancer drug targeted to a specific molecule on a specific cell type shown to extend survival. Gleevec, for example, worked so well against its initial indication of a type of leukemia that FDA approval took just about 3 months.
But Aduhelm (aducanumab) was approved only on evidence of it lowering levels of two biomarkers (amyloid-beta and tau protein) – not on clinical improvement, although those data are starting to roll in.
Here is the sobering conclusion of David Rind, MD, Chief Medical Officer of ICER, the Institute for Clinical and Economic Review, an independent source of drug review:
“The clinical trial history and evidence regarding aducanumab are complex. We have spent eight months analyzing the study results, talking with patient groups and clinical experts, and working with the manufacturer to understand their position. At the conclusion of this effort, despite the tremendous unmet need for new treatments for Alzheimer’s disease, we have judged the current evidence to be insufficient to demonstrate that aducanumab slows cognitive decline, while it is clear that it can harm some patients.”
Alzheimer’s disease is a slow process, and it’s possible that Aduhelm will indeed help. But demonstrating that will take more time.
The bottom line: the drug approval process is complex. It requires a bedrock of preclinical work, clinical trials carefully controlled to yield the most informative results, and a non-emotional approval process so that consumers can be certain that taking a new drug is backed with solid evidence of at least a chance that it might work.